Recent Posts
Psoriasis
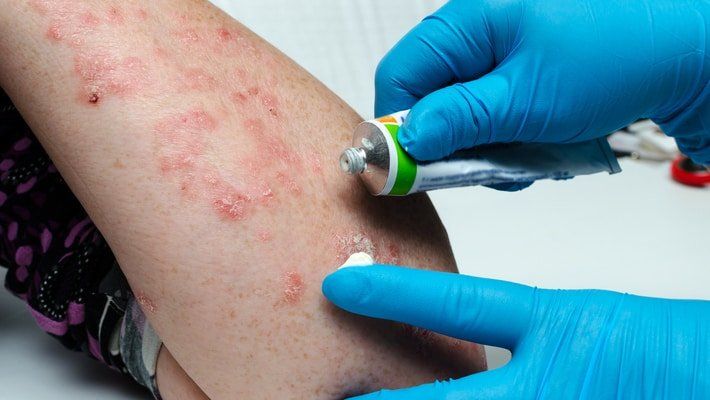
When it comes to skin rashes, the common perception is to think that they are the result of an allergic reaction. Sometimes, this is due to a personal care product. Other times, it could be caused by being exposed to specific foods, plants, or chemicals. But not all rashes are created equal, and not all of them can be soothed by applying a topical ointment and avoiding its triggers. In fact, for some people, skin changes are caused by things that are happening inside the body — such as autoimmune disorders. Such is the case with psoriasis. But, what, exactly, is it? How do you know if your skin changes are signs of psoriasis? And, what are the best treatment options?
What is psoriasis?
Psoriasis is a chronic skin condition that causes a person to develop red, itchy patches. These rashes occur due to your own autoimmune system attacking existing healthy skin cells and causing new skin cells to multiply at a faster rate. This creates excess skin that turns into thick, scaly areas — known as plaques — that typically appear on the knees, elbows, torso, and scalp. These plaques can become painful or cause a person to feel a burning sensation on the skin.
There are different types of psoriasis, and they are identified by the part of the body where they occur the most. While plaque psoriasis is the most common, some individuals can also experience:
- Nail psoriasis: This affects the area around the fingernails and toenails, and may cause abnormal nail growth.
- Inverse psoriasis: This type of the condition mainly affects wherever skin folds — such as under the breasts, groin, neck, and buttocks.
- Pustular psoriasis: This type of psoriasis is evident by pus-filled lesions on the plaques caused by plaque psoriasis.
- Psoriatic arthritis: This type of psoriasis cause the red, scaly, itchy patches to appear around the person’s joints.
- Erythrodermic psoriasis: This is the least common type of psoriasis, and it involves the rashes covering the entire body.
Psoriasis cycles through flare-ups and remission. While it can be managed and controlled with lifestyle changes, the condition has no cure.
Are there any factors that trigger psoriasis flare-ups?
A small percentage of people with psoriasis inherited the genes from one of their parents. The cause for the rest of the patients who live with psoriasis is unknown. However, the immune system can be triggered to attack healthy skin cells by several factors. The most common ones include:
- Excessive stress
- Having an underlying autoimmune disorder
- Suffering from an infection that weakens the immune system
- Excessive consumption of alcohol
- Smoking
- Certain medications
- Skin injuries
- Cold temperatures
What are the signs and symptoms of psoriasis?
Psoriasis is easy to identify due to the red, scaly patches of skin throughout the body. Depending on the severity of the condition, some people may only experience a few patches, while others may see them flare up on multiple parts of the body. In addition to the patches, other characteristics of these types of rashes include:
- Swollen joints
- Stiff joints
- Bleeding skin
- Silver or white scales on the red patches
- Thickened nails
- Skin soreness
Treatment Options for Psoriasis
You can soothe flare-ups with either oral or topical medications. Your doctor may also recommend injectable drugs to obtain relief from your symptoms. In addition, you can implement certain lifestyle changes to prevent flare-ups.
Take Care of Your Skin
Apply moisturizing lotions approved by your doctor when you’re indoors. Wear sunscreen and other protective clothing — such as sunglasses, hats, and long sleeves — if you’re going to be outdoors for extended periods of time.
Manage Stress
Stress causes inflammation in the body. If there are sources of stress in your life that cannot be avoided — such as an ill family member or demands at work — find ways to cope with it, whether by talking to a therapist, exercising, or meditating.
Eat a Healthy Diet
Being overweight or obese can exacerbate symptoms of psoriasis. Therefore, maintaining a healthy weight (a body mass index below 30) can help prevent or reduce flare-ups. You can start by reducing processed foods, staying hydrated, grilling foods instead of frying them, and cooking at home more often. You can also talk to your doctor or a nutritionist for a plan that works best for you.
Reduce Alcohol Intake
Consuming excessive amounts of alcohol triggers psoriasis flare-ups, makes symptoms worse and can have a negative effect on treatment. It also lowers your immune system. In addition, there’s a link between alcohol abuse and psoriasis.
If You Need a Virtual Medical Consult, Let Us Help You
At St. Hope, we serve many patients living with a myriad of medical conditions. We believe that treating people with compassion is as important as the medicine they receive. We foster a trusting patient/medical provider relationship to ensure that everyone who walks through our doors feels comfortable and receives the care they deserve — and we do so in-person and online.
We take same-day appointments, accept all insurance plans, and welcome walk-ins. Call us at 713-778-1300 or visit us at one of our five locations or schedule a televisit.